Tag: Health
-

Why Didn’t I Think of That? – Clare Riddell, Pressure Point
FHT’s annual Training Conference has officially started! We’re super excited for you to see what this year has to offer. Clare Riddell, has very kindly provided us with more information on herself and her practise for you to read before watching her webinar, ‘Why Didn’t I Think of That?’. Clare Riddell – Pressure Point I’d…
-

Snooze or Lose: Sleep-Inducing and Sleep-Disrupting Foods
While eating too soon before bed can damage your sleeping pattern, there are some foods and light snacks that can help you get a better night’s rest. Sleep experts at Bed Kingdom have revealed some foods with the perfect nutrients to help you enjoy a good night’s sleep.
-

Vitamins to Tackle Winter Blues
Winter blues, also known as Seasonal Affective Disorder (SAD), is a type of depression that occurs at a specific time of year, usually during the fall and winter months when there is less sunlight. While vitamins alone may not be a cure for SAD, certain vitamins and minerals play a role in maintaining overall mental…
-

Renewed Collaboration with Physique
We are delighted to share the exciting news of the revival of our collaboration with Physique Management, a distinguished name in the realm of sports healthcare products. For over 25 years, Physique has supplied therapists, medical professionals, elite sports teams and consumers with products that professionals trust in the most demanding situations. Their product lines…
-

Tips to Battle Blue Monday
Blue Monday, often dubbed the gloomiest day of the year, is the perfect opportunity to focus on elevating our mood, embracing joy and safeguarding our wellbeing. In this blog, Denise Lordache will explore practical strategies to counter the Monday blues while prioritising sleep and overall health. By Denise Lordache, sleep therapist & founder JoySpace Therapy…
-

Try something new in November
This months Action for Happiness calendar is ‘New Ways November’. As a holistic therapist, it’s key to promote wellbeing and balance in the lives of your clients. But how often do you apply the same principles? November, with its crisp air and transitional nature, provides the perfect backdrop for embracing change and trying something new.…
-

Non-Surgical Cosmetic Licensing Consultation FAQs
The new Health and Care Act 2022 gives the government powers to introduce a licensing scheme for practitioners who operate in England. Work is now underway to decide what the licensing scheme will look like, the first stage of this is a national consultation. The reason for the legislation is to reduce the risk of…
-
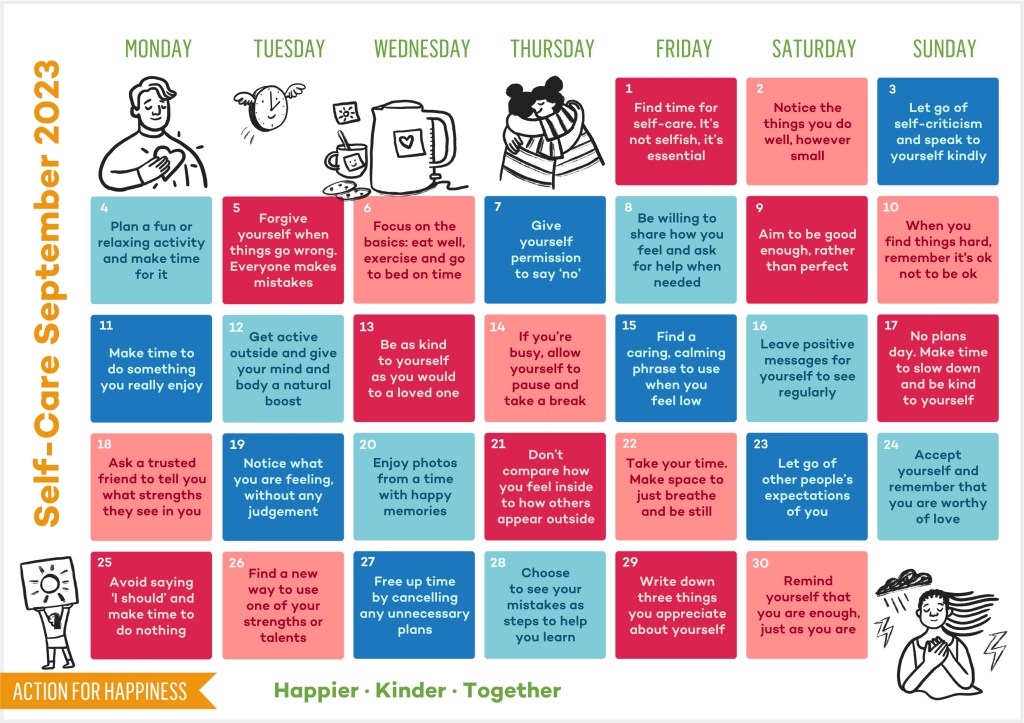
Embrace Self-Care September
As we transition into the autumn season, there’s no better time to focus on self-care and wellbeing. September is the perfect opportunity to embark on a journey toward happiness, and what better guide to accompany us than the Action for Happiness calendar? September often marks the return to routine after the carefree days of summer.…
-

Embrace Your Future with Holistic Health Apprenticeships
Are you ready to take the next step after your GCSEs? As results day approaches on 24 August, it’s time to consider the exciting opportunities that lie ahead. If you have a passion for holistic health and wellness, there are some fantastic apprenticeships waiting for you. From beauty therapy to wellbeing and holistic therapy, there’s…
-

Enhance Your Therapeutic Journey with FHT Local Support Groups
In the world of therapies, finding a community that shares your passion and supports your growth is invaluable. This is where local groups, supported by the FHT, come into play, offering a vibrant and nurturing environment for individuals who are dedicated to the field of therapies. These groups serve as more than just gatherings; they’re…
-

Love Parks Week 2023
Love Parks Week is happening from 28 July – 6 August 2023. Take this time to discover the power of nature and the profound impact that spending time outside can have on our wellbeing. It’s the perfect opportunity to reconnect with the wonders of wildlife and experience its transformative benefits. Here, we list three ways…

